The Link Between Periodontics And Implant Success
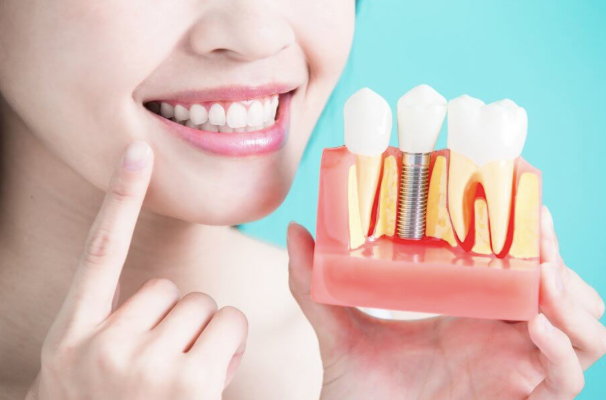
Healthy gums decide if your implant lasts or fails. Periodontics is the care and treatment of your gums and bone. These tissues hold your implant in place. When they break down, the implant loses support and can loosen or fall out.
This blog explains how gum disease harms implants, how a periodontist protects bone, and why early treatment raises success. You will see how deep cleanings, gum surgery, and steady home care all shape the life of your implant.
You also learn what to ask your provider before surgery, and how to spot warning signs after. Pain, bleeding, and bad breath are not small issues. They can signal early implant trouble.
If you are considering dental implants Queens or already have one, understanding periodontics gives you control. Strong gums are not extra care. They are the base of every successful implant.
Why your gums control implant success
Your implant is a metal post in your jaw. Your bone grows around it. Your gums seal around it. Together they form a barrier that keeps out germs and pressure.
When gums swell or pull away, that barrier opens. Germs reach the bone. The bone starts to shrink. The implant loses grip. Many failed implants start with quiet gum problems that go unchecked for months.
Periodontics focuses on three things that protect your implant.
- Removing sticky plaque and hard tartar
- Stopping bone loss from infection
- Guiding you on daily care that keeps gums calm
How gum disease threatens implants
Gum disease starts with plaque at the gumline. Plaque holds bacteria that cause redness and bleeding. If you do not remove it, it hardens into tartar. Then the infection moves deeper.
Around natural teeth, this process is called periodontitis. Around implants, it is called peri-implantitis. The process is similar. The result is the same. Bone disappears.
The National Institute of Dental and Craniofacial Research explains how plaque and tartar cause gum disease and bone loss around teeth.
Key warning signs include three changes.
- Bleeding when you brush or floss
- Swelling or a puffy look around the implant
- Bad taste or odor that does not go away
Later signs include pain when chewing and implant movement. At that stage, saving the implant is much harder.
Natural teeth versus implants
Implants act like teeth. They are not the same as teeth. The way gums attach is different. This difference makes implants more prone to fast damage once infection starts.
| Feature | Natural tooth | Dental implant |
|---|---|---|
| Support structure | Root with ligament fibers | Titanium post fused to bone |
| Gum attachment | Strong fiber network into root surface | Weaker seal around smooth metal or ceramic |
| Response to plaque | Slow bone loss in many cases | Bone loss can progress faster |
| Nerve sensation | Has nerves that warn you of pressure | No internal nerve sensation |
| Main risk without care | Loose tooth and tooth loss | Implant failure and removal |
This is why strict gum care is not optional after implant surgery. It is part of the treatment itself.
How a periodontist protects your implant
A periodontist is a dentist who focuses on gums and bone. Before implant surgery, this expert looks for silent problems that could shorten implant life.
The visit often includes three steps.
- Review of your health, medicines, and smoking history
- Gum measurements to check pocket depth around teeth
- X-rays to measure bone height and shape
If gums or bone show damage, treatment comes first. That can include deep cleaning under the gums and medicine in the pockets. In some cases, you may need bone grafting or gum grafting to build a strong base.
The American Academy of Periodontology explains how gum disease and peri-implantitis are treated using deep cleanings, local medicine, and surgery.
Your role before and after surgery
You share control of implant success with your provider. Your daily actions can protect the work done in the clinic.
Before surgery, ask three direct questions.
- Do I have any gum disease now
- Is my bone thick enough and strong enough
- What habits do I need to change before surgery
Smoking, poor blood sugar control, and dry mouth each raise risk. Your provider can help you plan small changes that lower that risk.
After surgery, focus on these simple habits.
- Brush twice each day with a soft brush at the gumline
- Clean between teeth and implants once each day with floss or small brushes
- Use any rinse or tool your periodontist suggests for your case
Schedule checkups at the pace your provider sets. Many people with implants need cleanings every three to four months. These visits catch small changes early when care is easier and less costly.
See also: Home Health Care Explained: Services, Benefits, and What to Expect
Warning signs you must not ignore
Some changes around an implant need fast attention. Call your provider if you notice any of the following signs.
- Bleeding during brushing that repeats for more than two days
- Swelling, a bump, or pus near the implant
- New space between the implant crown and neighboring teeth
- Change in how your bite feels when you close
- Any movement of the implant post
Quick treatment can stop bone loss and keep the implant in place. Waiting out the problem often leads to more pain and more complex surgery.
Building a long lasting smile
Implants can restore chewing, speech, and confidence. Yet they only stay strong when gums and bones stay healthy. Periodontics links these pieces together.
When you treat your gums as the base of your implant, you protect both your health and your investment. You also give your family a model of steady, quiet self-care. Strong gums, careful cleaning, and regular visits form a simple rule of three that supports every implant for many years.